- More Than Teeth
- Posts
- Airway Healing Beyond the Mask: Case Study of Jill’s Journey
Airway Healing Beyond the Mask: Case Study of Jill’s Journey
Where Dentistry Meets Whole-Body Health Michael Bennett, DDS, PhD & Cathy Bennett, MS, NBCHWC
Good morning. This is More Than Teeth. The newsletter that helps dental sleep professionals get 1% better every week.
Good Morning,
For many patients, CPAP is life-saving. But for some, it’s also life-limiting.
Masks irritate skin. Pressure worsens pain. And for kids, CPAP can miss the root cause altogether. CPAP is a bridge, not a destination.
Today’s story from Dr Bennett illustrates why you matter as a dentist in sleep medicine—and why oral appliance therapy can restore health, dignity, and even careers.
In Today’s Issue
Dr Bennett’s Case Study: Jill’s journey beyond CPAP
The limitations of CPAP therapy
Oral appliance therapy (OAT) as a restorative, growth-friendly solution
Dissertation lens: Role clarity improves acceptance and referrals
Cathy’s Corner: Inflammation and CPAP pressure
Business of Sleep: Reviewing referral and follow-up systems
5-minute read👇
Clinical Corner
🥼Use the clinical corner as your secret weapon to impress your colleagues and patients!
Key Takeaways
-CPAP works in theory—but often fails in practice due to poor compliance, high pressure, and patient discomfort
-Oral appliance therapy can open the airway while reducing pain, improving sleep, and restoring life quality
-Clear dentist-physician collaboration improves referral pathways and case acceptance
-Inflammation makes CPAP harder to tolerate—addressing nutrition and lifestyle supports therapy success
-Reviewing your referral and follow-up process is a simple way to elevate care this week
Case Study: When CPAP Isn’t the Lifeline
Meet Jill (name changed).
At 52, this former nurse came to us desperate for answers. She had tried CPAP. She needed CPAP. But her reality?
Severe skin sensitivity made the mask unbearable
Leaks and pressure aggravated her TM joint pain
Mandibular pain from even slight pressure
Struggles with obesity, diabetes, heart failure, and fibromyalgia
She was drowning in symptoms—and had already left her beloved nursing career because her body couldn’t keep up.
The Problem: CPAP was working in theory but failing in practice. For Jill, it wasn’t a lifeline—it was a barrier.
Exploring Alternatives
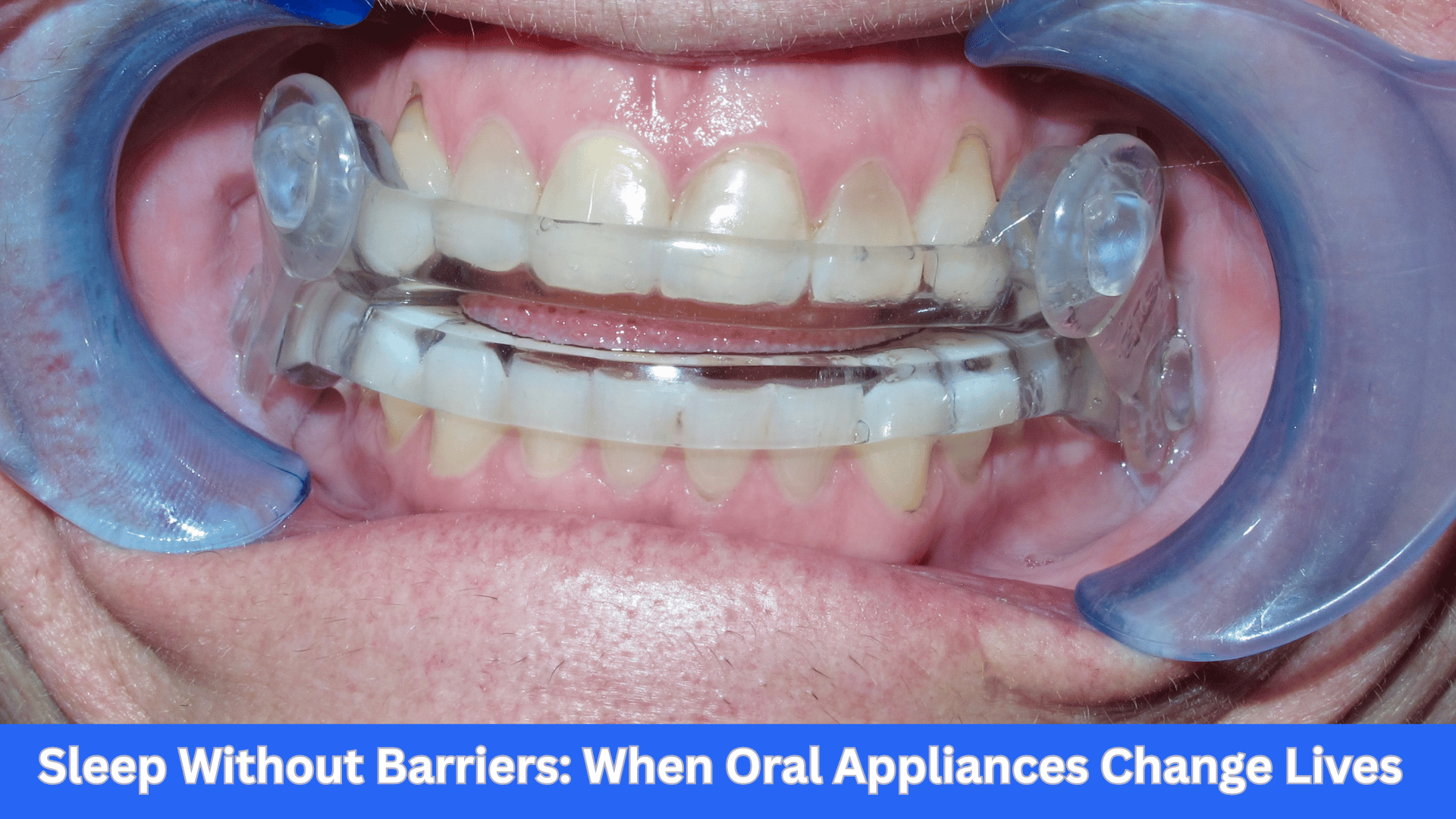
Instead of giving up, Jill wanted to explore an advanced oral appliance option. Despite missing second molars, we collaborated with our lab to create a custom EMA:
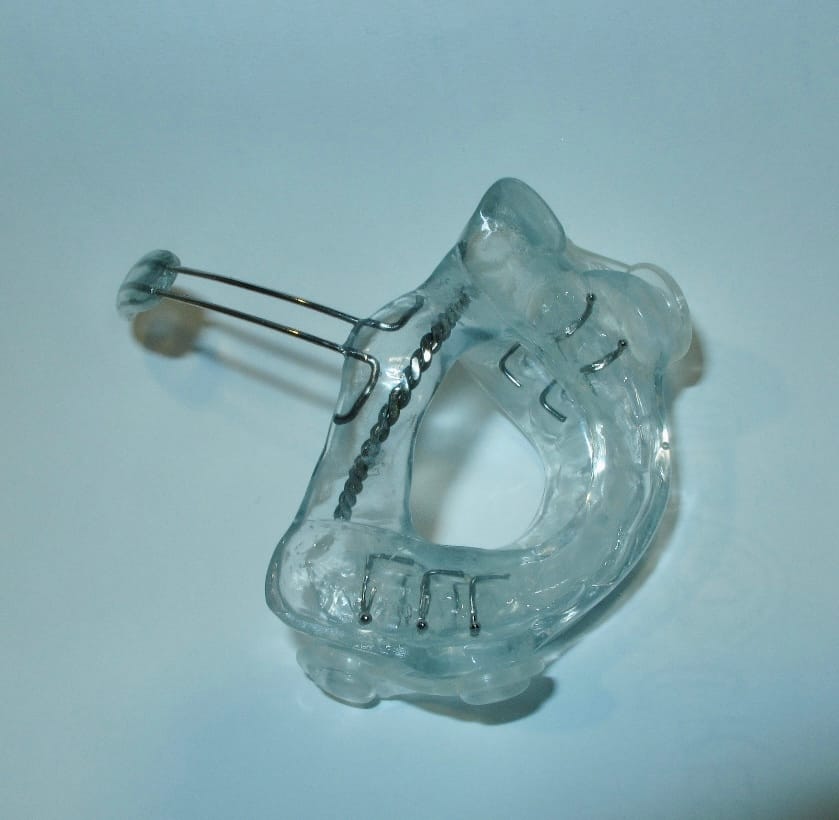
Custom EMA
A tongue extension, crafted with wire and acrylic
Positioned in the functional space between the soft palate and lingual tonsils
Designed to stabilize her airway without compressing the mandible
Yes, there was a risk—her gag reflex. But Jill was determined to try.
The Turning Point
With careful adjustments—and added nasal protocols to clear congestion and reduce gag sensitivity—something remarkable happened:
Jill got used to the device. She started sleeping well at night, felt less pain, and had more energy. The best part was that she could go back to her nursing job, which she loved, and worked for several more years with better health and confidence.
Proof in the Scan
Her sagittal CT scans told the story best:
Before: a constricted airway, correlating with fragmented sleep and pain
After appliance: a measurably open airway, matching her improved symptoms and restored vitality
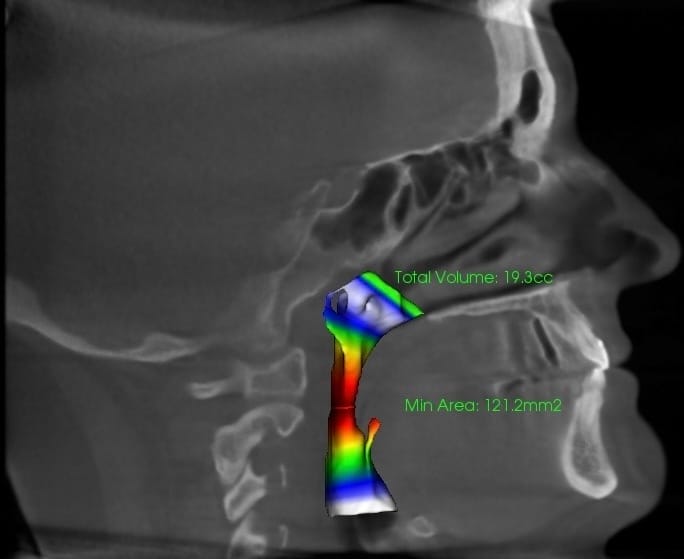
Before appliance
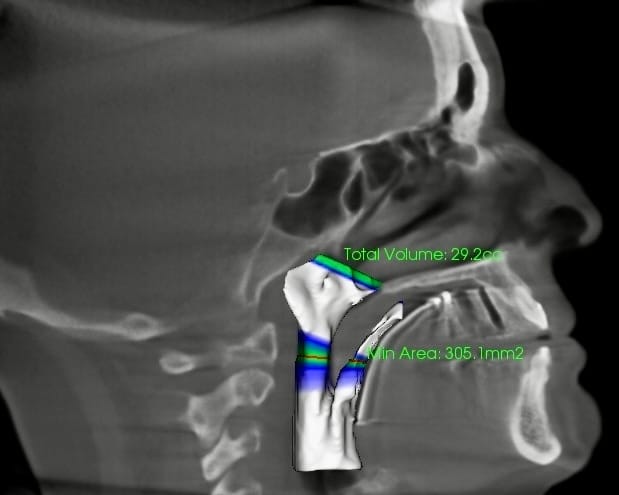
After appliance
The Problem With CPAP (and Why You Matter)
CPAP is essential—but incomplete.
For many patients, CPAP masks become nightstand dust collectors. Poor fit, dryness, noise, and high pressures all chip away at compliance. Even when tolerated, CPAP doesn’t correct underlying structural and inflammatory issues.
Children are often missed altogether.
A child with crowded teeth, dark circles, and restless sleep may be started on CPAP, when in reality, their jaw growth, airway development, or nasal inflammation should be addressed.
This is where dentistry makes the difference.
OAT provides a restorative, growth-friendly alternative for children and a pressure-reducing adjunct for adults already on CPAP. When dentists screen, identify, and communicate clearly with physicians, patients win.
Dissertation lens: Dr. Bennett’s research found that role clarity—the ability for dentists to explain “here’s where I fit in”—improves both case acceptance and referral quality. Patients are more likely to say yes when they understand how CPAP and OAT can work together instead of competing.
Research Spotlight
Jill’s custom oral appliance worked because we could think beyond the mandible and focus on tongue position. For her, a tongue extension added to an EMA stabilized her airway without overloading her TM joint.
New research is exploring this very concept. A 2023 clinical trial protocol by Fukuda et al., Control of Tongue Position in Patients with Obstructive Sleep Apnea, is testing whether holding the tongue in a resting or protruded position can reduce apneic events compared to no tongue control. Their work supports what Jill’s story illustrates: sometimes, the key isn’t just moving the jaw—it’s guiding the tongue to maintain airway patency.
This growing body of research validates the clinical creativity required when CPAP fails and standard appliances aren’t enough. It reinforces that dentists play a critical role in customizing airway solutions that change lives.
Cathy’s Corner: Inflammation and Pressure
“When the body is constantly inflamed, it doesn’t respond well to sleep pressure.”
CPAP may deliver air, but inflamed tissues and immune imbalance mean the body can’t heal under pressure alone. By reducing dietary inflammation—sugar, alcohol, processed foods—patients often find both CPAP and OAT more tolerable and more effective.
The Business of Sleep
Dentists thrive when they have clear systems for referral and follow-up. Ask yourself:
Do you track whether referred patients actually tolerate CPAP?
Do your medical colleagues know you offer co-therapy to reduce pressure needs?
Is your referral form worded to build trust (e.g., “supportive therapy” vs. “alternative”)?
Action Step: Review your current referral and follow-up process this week. Even one small change can elevate case acceptance and strengthen physician partnerships.
CE Opportunities / Events
Event | Dates | Location | Link |
|---|---|---|---|
AADSM Mastery Program | Ongoing dates (check website) | Online | Click HERE |
Transform Your Practice with Dental Sleep Medicine | October 17-18, 2025 | Tempe, AZ | Click HERE |
Dentist’s Role in Snoring & Sleep Apnea | November 7-8, 2025 | Chicago, IL | Click HERE |
Have an event you would like to post? (free) [ click here ]
Miscellaneous
After one year, about half of the people using CPAP machines continue to use them regularly. Oral devices can often lower the pressure needed from CPAP machines by up to 40%. For children, it's better to help their airways develop naturally with myofunctional therapy, nasal clearing protocols, and airway orthodontics for a permanent solution rather than using masks.
CPAP saved Jill, but it wasn’t her forever. Dentistry gave her another chance.
Remember: you’re not competing with CPAP—you’re completing the care.
With you in the movement,
Mike & Cathy

Reply